
Introduction
Patient misidentification and healthcare data breaches represent critical vulnerabilities in modern hospitals. An ECRI Institute study classified over 7,600 out of 10,915 events as wrong-patient incidents involving patient identification errors between January 2013 and August 2015. These errors trigger duplicative testing, unsafe treatments, and financial losses through denied claims.
Biometrics address these risks directly. Hospitals in 2026 are moving beyond passwords and ID cards, adopting contactless verification to secure facilities, authenticate staff, and confirm patient identity at the point of care.
Post-COVID infection-control requirements accelerated this shift — hygiene-compliant solutions are no longer optional. What follows covers the top biometric identification features to evaluate in 2026, ranked by accuracy, hygiene, speed, and fit with clinical workflows.
TL;DR
- Biometric identification solves patient safety and facility access control simultaneously
- Top modalities for 2026: palm vein, facial, iris, fingerprint, and voice recognition
- Key criteria: accuracy rate, contactless capability, verification speed, EHR integration, HIPAA compliance
- Palm vein scanning tops the list for hospitals — contactless, 99.99991% accurate, and verified in under 2 seconds
- Choosing one platform for both patient ID and staff access reduces integration costs and compliance complexity
Overview of Biometric Identification in Hospital Technology
Biometric identification in hospitals uses unique physiological or behavioral traits to verify patient and staff identity, replacing or supplementing traditional credentials like ID badges, PINs, and passwords.
Biometrics serves two distinct roles in healthcare environments:
- Patient registration and treatment checkpoints — reduces misidentification at medication dispensing, lab draws, and surgical prep, where a wrong-patient error can be fatal
- Staff access control — restricts entry to ICUs, pharmacies, server rooms, and EHR systems to verified personnel only
- Audit trail generation — creates timestamped, identity-verified records that satisfy HIPAA access logging requirements
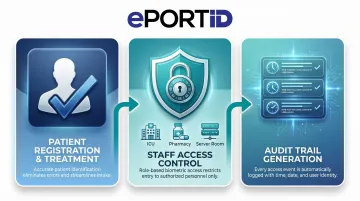
Together, these applications make biometric authentication a compliance necessity, not an optional upgrade, heading into 2026.
The healthcare biometrics market reflects this urgency. According to a 2024 report by MarketsandMarkets, the healthcare biometrics market is projected to reach $14.5 billion by 2025, driven by rising medical identity theft and stricter patient data regulations. Hospitals are treating biometric infrastructure as essential — not aspirational.
Best Biometric Identification Features in Hospital Technology 2026
These five biometric modalities were evaluated on accuracy, contactless capability, speed, liveness detection, EHR/HRIS integration, and suitability for clinical environments.
Palm Vein Recognition
Palm vein recognition scans the unique subcutaneous vein pattern in a person's palm using near-infrared light. This approach makes it inherently contactless, impossible to duplicate, and resistant to spoofing—veins are internal and only readable in living persons.
Solutions like ePortID, powered by Fujitsu technology, deliver 99.99991% accuracy from 5 million data points in under 2 seconds—a pattern unique to every individual, including identical twins. The system checks for liveness during verification by detecting blood flow beneath the skin surface, preventing presentation attacks using photographs or replicas.
Why palm vein excels in hospitals:
- No physical contact with hardware—critical for infection control
- Immune to surface damage affecting fingerprints
- Works consistently across demographic groups
- Integrates with access control and time-attendance systems
- Eliminates buddy punching and unauthorized entry to restricted areas
| Feature | Specification |
|---|---|
| Accuracy | 99.99991% (Fujitsu-based solutions like ePortID) |
| Verification Speed | Under 2 seconds per verification |
| Best Hospital Use Cases | Staff access control (ICU, pharmacy, server rooms), time and attendance, patient identity at high-security checkpoints |
Facial Recognition
Facial recognition uses AI-driven analysis of facial geometry to identify individuals. Its widespread hospital adoption for patient onboarding at registration desks, self-service kiosks, and outpatient clinics stems from its fully hands-free nature. Leading systems include liveness detection to prevent photo spoofing.
Top-ranked facial recognition systems evaluated by NIST achieve high match rates and integrate with EHR platforms for real-time patient identification. NIST research shows wide-width masks produce false negative rates about 1.6 times higher than rounder masks—a relevant concern in clinical environments where protective equipment is routine.
Where facial recognition fits in hospitals:
- Fully hands-free patient onboarding at registration and kiosk points
- Fast emergency department check-in without staff assistance
- EHR-integrated identification at controlled entry points
- Best suited to low-PPE areas; mask-wearing meaningfully raises false non-match rates
| Feature | Specification |
|---|---|
| Accuracy | High match rates from NIST-evaluated systems; mask-wearing significantly increases false non-match rates |
| Verification Speed | Typically 1–3 seconds |
| Best Hospital Use Cases | Patient registration/onboarding, emergency department check-in, controlled entry points |

Iris Recognition
Iris recognition maps the unique patterns of the iris using infrared imaging. It is contactless, highly stable over time, and widely regarded as one of the most accurate biometric methods available. Hospitals deploy it for patient identification where preventing duplicate records and medical identity theft is the priority.
Iris-based systems have demonstrated rapid deployment (operational within days), high patient acceptance rates, and the ability to maintain a clean Master Patient Index (MPI)—a critical metric for EHR data integrity and patient safety. However, initial deployments may experience high false reject rates due to high image contrast between the sclera and surrounding skin tone, requiring threshold tuning for optimal performance.
Why hospitals use iris recognition for patient identity:
- Contactless and stable—iris patterns don't degrade with age or skin condition
- Maintains a clean Master Patient Index, reducing duplicate record risk
- Supports medication dispensing authorization at the point of care
- Requires threshold tuning for optimal performance across skin tone variations
| Feature | Specification |
|---|---|
| Accuracy | Among the most accurate modalities; requires algorithm tuning for demographic variables |
| Verification Speed | Typically 2–4 seconds for clinical systems |
| Best Hospital Use Cases | Patient identity verification at medication dispensing, duplicate record prevention, insurance fraud prevention |
Fingerprint Recognition
Fingerprint recognition remains the most widely deployed biometric modality globally due to its cost-effectiveness and maturity. Hospitals use it for staff login to EHR systems, controlled room access, and medication cabinet authorization. Sensor miniaturization has made integration into clinical workstations straightforward.
Key limitation for hospitals: Fingerprint sensors require physical contact with a scanner surface, creating hygiene and cross-contamination risks. Studies have recovered S. aureus, Acinetobacter, Escherichia coli, and Pseudomonas species from biometric attendance devices in healthcare premises. This has made healthcare organizations increasingly favor contactless alternatives, particularly post-COVID.
Additional clinical challenges include sensitivity dropping below 15% for children under 13 and a 26% failure rate in capturing fingerprints in some hospital settings.
| Feature | Specification |
|---|---|
| Accuracy | Mature technology with reliable performance in ideal conditions; 26% failure rate documented in some clinical settings |
| Verification Speed | 1–3 seconds typical |
| Best Hospital Use Cases | EHR workstation login, medication cabinet access, administrative time tracking |

These contact-based limitations are pushing more clinical facilities toward hands-free alternatives—including emerging voice-based authentication.
Voice Recognition
Voice recognition identifies individuals through unique vocal patterns and is increasingly used in hospital settings for hands-free authentication. Its primary use case is enabling clinicians to log into EHR systems or authorize actions while maintaining sterile field conditions during procedures.
Background noise limits where it works reliably. Hospital alarms, patient activity, and busy ward environments all degrade accuracy, restricting voice authentication to specific low-noise workflows. AI-enhanced models are narrowing this gap, positioning voice as a useful secondary factor in multi-modal biometric setups rather than a standalone solution.
| Feature | Specification |
|---|---|
| Accuracy | Variable depending on background noise levels; improving with AI-enhanced models |
| Verification Speed | Typically 2–5 seconds for authentication |
| Best Hospital Use Cases | Hands-free EHR access in sterile environments, telehealth authentication, administrative phone-based verification |
Key Benefits Driving Biometric Adoption in Hospitals
Patient Safety and Fraud Prevention
Biometric identification directly reduces patient misidentification errors at critical checkpoints—medication dispensing, surgery, lab results. It also prevents medical identity theft and insurance fraud, two risks that paper-based or card-based systems handle poorly.
AHIMA reports the average duplication rate in healthcare is between 8 and 12 percent. These duplicate records force hospitals to spend hundreds of thousands of dollars every few years with outside vendors to reconcile records. Biometric patient identification eliminates this recurring cost while preventing the clinical dangers of merged or overlaid medical records.
Operational Efficiency and Payroll Integrity
Biometric attendance systems eliminate buddy punching, create auditable time-and-attendance records, and reduce payroll processing overhead. Well-implemented systems can pay for themselves within 3 to 6 months through recovered labor costs and reduced administrative burden.
For shift-based healthcare workers, rapid authentication (under 2 seconds) prevents bottlenecks during busy shift changes while maintaining accountability that traditional ID cards or PIN codes cannot provide. That same accountability extends directly into regulatory compliance—where the audit trail a biometric system creates can mean the difference between a clean review and a costly violation.
Regulatory Compliance and Audit Readiness
Biometric systems generate timestamped access logs that support HIPAA compliance, controlled substance tracking, and facility security audits. Systems must handle biometric data carefully to meet regulatory standards.
Look for solutions that:
- Store biometric data as encrypted mathematical templates, not raw images
- Support the "right to be forgotten" for patient and employee data
- Keep biometric templates separate from personally identifiable information
- Meet HIPAA requirements and, where applicable, GDPR data handling standards
How We Chose the Best Biometric Identification Features
Our evaluation framework focused on documented real-world performance in clinical environments — not just lab benchmarks. Each feature was scored across these criteria:
- Accuracy rate — false acceptance and false rejection rates under clinical conditions
- Contactless capability — critical for infection control in patient-facing settings
- Verification speed — measured in active clinical workflows, not controlled demos
- Liveness detection — resistance to spoofing and presentation attacks
- EHR/HRIS integration — compatibility with existing hospital systems
- HIPAA compliance — regulatory alignment verified, not assumed
Common healthcare buyer mistakes:
- Prioritizing upfront cost over total cost of ownership
- Choosing contact-based systems without considering infection control implications
- Selecting single-modality solutions that fail in edge cases (masks, gloves, background noise)
- Overlooking liveness detection against presentation attacks
Multi-modal biometric solutions using two factors demonstrate 97.4% authentication success rates compared to 91.8% for single-modality systems, reducing authentication failures by 72.3% in clinical environments.
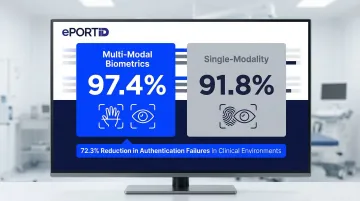
The right biometric solution for a hospital is the one that fits your specific use case — patient ID, staff access control, or both — integrates cleanly with existing systems, and delivers measurable results within months of deployment. Price and brand recognition are secondary to that fit.
Conclusion
Biometric identification in hospitals has moved from pilot phase to operational standard by 2026. Palm vein, facial, iris, fingerprint, and voice recognition each serve distinct roles—the right choice depends on the hospital's priorities: contactless hygiene, patient safety, staff access control, or EHR security.
When evaluating options, healthcare decision-makers should look beyond accuracy on paper. Three factors consistently separate deployments that work from those that don't:
- Performance in clinical conditions (gloved hands, high-traffic entrances, variable lighting)
- Scalability across departments without reconfigurations or hardware changes
- Vendor experience in regulated, high-stakes environments where failure carries real consequences
ePortID's palm vein scanning platform was built against exactly those standards. The company's background spans 20 years securing US Navy bases, Army JTF installations, and port authorities—environments where access failures aren't recoverable. That experience, combined with Fujitsu's scanning hardware and 99.99991% identification accuracy at under two seconds, translates directly to hospital settings: restricted wards, server rooms, pharmacy access points, and patient check-in. For facilities that need a contactless solution with a documented deployment record, it's a substantive starting point.
Frequently Asked Questions
Frequently Asked Questions
Which biometric technology is best for hospitals?
No single modality wins across every use case. Palm vein and iris recognition lead for high-security patient identification due to contactless operation and near-perfect accuracy, while facial recognition excels for high-volume patient onboarding. Match the technology to your hygiene requirements, environment, and existing infrastructure.
What are the future trends in biometrics for healthcare?
The dominant 2026 trends are:
- Multi-modal biometrics combining two modalities for redundancy
- AI-enhanced liveness detection to prevent spoofing
- Deeper EHR integration with real-time identity verification
- A broad shift from contact-based to contactless modalities driven by infection control standards
What biometric system is used in hospitals?
Hospitals use a mix of systems: iris and palm vein scanners for patient identification and high-security access, facial recognition for onboarding kiosks, and fingerprint readers for staff workstation login. Most facilities are migrating toward multi-modal platforms that combine two or more of these.
How is biometric data protected in healthcare settings?
Biometric data is stored as encrypted mathematical templates (not raw images), governed by HIPAA in the US, and subject to strict access controls. HIPAA-compliant systems support the "right to be forgotten" and do not store personally identifiable information alongside biometric templates.
Can biometric systems integrate with EHR platforms?
Leading biometric patient identification platforms integrate with major EHR systems — including Epic and Cerner — via APIs, enabling real-time identity verification at registration, medication dispensing, and treatment checkpoints.
How accurate are biometric systems in hospital environments?
Accuracy varies by modality and environment. Palm vein recognition achieves up to 99.99991% accuracy. Iris recognition and facial recognition from top-tier vendors approach similar levels in controlled conditions. However, clinical capture failures occur in edge cases — fingerprint sensitivity drops below 15% for children under 13, and facial recognition accuracy decreases significantly when patients wear masks.


